Epidemics in Ireland – A Short History
 By John Dorney
By John Dorney
At the time of writing, (March 30 2020), Ireland is in lockdown. Almost all normal work and social activity has been suspended in an effort to slow the progress of the coronavirus pandemic.
We have found ourselves in the novel and uncomfortable position of watching the spread of a virus to which no one has any immunity and for which there is at present, no vaccine. Not since the great flu epidemic of 1918-19 has Ireland (or most other European countries) faced anything of this nature.
Epidemics have occurred throughout human history.
However, epidemics of infectious diseases was something our ancestors faced at regular intervals over the centuries. While they had no clear idea of the nature of such diseases and usually no effective treatment, their measures to combat them might give us some lessons for our current predicament.
This article can of necessity be no more than a sketch, but it aims to give an outline of the most destructive epidemics in Irish history and how they were increasingly effectively countered from the mid 19th century onwards.
If there is a common thread running through centuries it is this: in the absence of a vaccine, the most important measures are vigilance, rapid identification of the infected and their isolation from the healthy population, and good general standards of hygiene.
The Black Death 1348-49 and bubonic plague

Plagues and epidemics are older than recorded history. The suburb of Tallaght in Dublin, for instance is thought to have been named Tamhlacht, ‘plague monument’ after some long forgotten pre-historic pestilence.[1]
However this article will begin with Ireland’s experience of the ‘Black Death’ the terrible bubonic plague that is thought to have killed up to 40 per cent of Europe’s population in the 14th century.
The bubonic plague is a bacterial infection spread by the fleas that live on rats and easily transmitted to humans, especially in densely populated unhygienic urban settlements.
The Black Death may have killed up 40 of the populations Ireland’s towns in he 14th century and crippled the medieval English colony.
It arrived in Ireland via the eastern ports in the summer of 1348, probably with traders from the French port of Bordeaux, and proceeded to cut a swathe through the population of eastern towns such as Dublin and Drogheda. It is thought to have arrived separately to southern port cities such as Cork and Waterford, from England, but the result was the same; an ‘unheard of mortality’ throughout the mostly English speaking urban settlements.
One Dominican Friar in Kilkenny, John Clynn, famously wrote, before his own death from the plague that he hoped that ‘one son of Adam’ might survive the pestilence. [2]
Accurate figures are impossible to come by for the medieval period, but it is estimated that the towns lost between 45-50 per cent of their inhabitants as a result of the Black Death and their rural hinterland was also devastated, with a shortage of famers and workers for generations afterwards. What was more, the plague recurred several more times in the 14th century.
While the Gaelic Irish were less affected, due to living mostly in more dispersed rural settlements, they too suffered, as their annals tell us of several notable clerics and noblemen who died. Nevertheless, one of the long term effects of the Black Death in Ireland was the near collapse of the English colony, the resurgence in political power of the Gaelic Irish and the retreat of the English presence into a fortified ‘Pale’ around Dublin.[3]
Even in the 16th century, plague epidemics regularly blighted Ireland. According to Colm Lennon, plague outbreaks occurred six times in that century. The last, from 1600-1604, coincided with the final phase of the Nine Years War, and plague, war and famine may together have carried off as much as 10% of the Irish population. [4]

War, famine and plague again conspired to cause mass mortality in the 1650s, during the Cromwellian conquest of Ireland. Plague, thought to have been brought to Ireland with the New Model Army, again killed in extraordinary numbers.
In the siege of Limerick for instance, in 1651, one in five of the city’s garrison and inhabitants died of the plague by the time the town surrendered to the Parliamentarian forces. Their commander Henry Ireton also succumbed to the plague. Estimates of the mortality in the Irish population in the 1650s vary between 10 and 40 per cent.
All of these calamities occurred well before the germ theory explained that diseases were carried by microorganisms – the most popular medical view up to the early 19th century was that they were carried by ‘miasmas or ‘vapours’ – ‘bad air’. Nevertheless, people in medieval and early modern Ireland did understand that diseases could be transmitted from person to person and that the sick must be kept segregated from the healthy.
All towns for instance had ‘leper houses’ outside their walls where sufferers of leprosy were kept segregated. During times of plague certain officials were designated to isolate victims and to bury the dead. Town watchmen had to scan those entering the walls for signs of sickness and others had to monitor the water and food supplies for the ‘taint’ of infection.[5]
Nineteenth century epidemics

By the dawn of the nineteenth century, bubonic plague was no longer the most dangerous epidemic disease in Ireland, though there were plague scares even as late as 1900.
Rather the biggest killers were now typhus, cholera, typhoid and dysentery.
Such fevers, especially typhus, which was spread by lice and therefore encouraged by unwashed bodies and clothes in close proximity to each other, had been the ‘scourge of Ireland’ for many centuries.
One Cromwellian soldier in the mid seventeenth century had called it, ‘malignant fever’ and said it was ‘commonly accompanied with a great pain in the head and in all the bones, great weakness, drought, loss of all manner of appetite, and want of sleep, and for the most part idleness or raving, and restlessness or tossings, but no very great nor constant heal’. [6]
Cholera is thought to have been introduced to Ireland from India, probably via British troops. Cholera is a bacterial infection caused by water and food contamination. Acute, sudden diarrhoea can cause severe hydration and death. Typhoid (not to be confused with typhus) similarly was caused by drinking unclean water.
Epidemics were regular and lethal in the 19th century; the biggest killers were typhus, cholera, typhoid and dysentery.
And added to the lethal mix was smallpox, an acute viral disease which was (like Covid 19) generally transmitted by airborne droplets. Smallpox, in severe cases, caused internal bleeding that could cause rapid death, and a characteristic rash that could cause blindness and infertility in survivors and even in mild cases, a scarred, pockmarked face.[7]
A typhus epidemic in 1816-17 killed over 65,000 people out of over 1.5 million infected, one of six such epidemics in the 19th century, while an outbreak of cholera in the 1830s killed another 50,000 people. [8]
During the Great Famine of the 1840s, hunger and malnutrition-related diseases claimed a large proportion of the over 1.5 million victims, but typhus or ‘famine fever’ killed at least 400,000 of them. [9] As medical historian Laurence Geary writes, ‘The relationship between famine and fever is complex, but there is no direct nutritional connection.’[10]
As many as one third of the victims of the Great Famine died due to ‘fever’ or epidemic disease.
In other words, many died not of starvation but of ‘fever’ when the destitute left their homes and packed into overcrowded towns, prisons and workhouses where hygiene was bad and the lice which transmitted typhus could spread easily, as could smallpox which was transmitted from person to person by respiratory droplets.
One observer wrote, somewhat unkindly given the rational fears of the populace, ‘the horror of contagion among the Irish poor amounts in general to a perfect monomania [obsession]’.[11]
Over 200 doctors died during the famine, mostly of epidemic disease. However their sacrifice may have been futile, given the state of medical knowledge at the time. As historian of the famine Cormac O Grada writes, ‘medical help was of little benefit when not positively harmful’. ‘Treatments’ included bleeding, by cutting or application of leeches, proscribing whiskey, laudanum (a derivative of opium), mercury or even chalk. O Grada judges that ‘medical treatment is unlikely to have saved many lives during the famine’.[12]
Dealing with epidemics in the 19th century

If treatment of epidemic disease remained primitive, there was, however, some progress in what is now termed the ‘non-pharmaceutical intervention’ in epidemics.
The first of these was vigilance, Dr Patrick Rowan writes: ‘Following the 1817 typhus epidemic, a Fever Act was passed the following year which allowed mayors of towns to prevent strangers entering their towns when fever was prevalent.’[13]
The second was isolation of the infection. During the 1816-17 typhus epidemic and again during the Great Famine, hundreds of temporary fever hospitals were established to care for the sick and, just as important, to segregate them from the healthy to limit the spread of infection. Between Poor Law Unions or Workhouses and County Hospitals over 100 permanent fever hospitals had also been established by the 1840s and more followed after 1851.
Though medical care remained primitive until the mid nineteenth century, great strides both in hygiene and treatment were made thereafter.
The poor quite rightly feared these fever hospitals as sites of infection and many local government bodies lobbied not to have them located in their towns. When, during the Great Famine, fever hospitals were overrun with patients, the overflow of patients was accommodated in wooden sheds and tents, where the mortality was fearfully high.
Cork Street Fever Hospital in Dublin, for instance, admitted 14,700 patients in one month alone, March 1847, during the famine. The wealthier preferred to quarantine their sick loved ones at home if at all possible.[14]
But for all that, these fever hospitals did probably save lives by reducing the risk of those sick with ‘fever’ infecting those patients suffering from other malnutrition-related illnesses.
Typhus began to decline as a big killer in the second half of the nineteenth century. The acceptance of the germ theory of disease helped to improve the understanding of the importance of hygiene and though anti-biotics were still a long way in the future (they only became widespread in the 1930s), measures such as boiling water and using soap for washing clothes, bodies and hospital surface made a big difference to hygiene in hospitals and elsewhere.
That said, there were still outbreaks of typhus in early 20th century Ireland notably in Connemara in 1913. Poverty and the squalid conditions of many poor urban areas in Ireland (particularly the Dublin slums) meant that typhus was not totally eradicated in Ireland until the 1940s.
Similarly the advent of sanitation and clean drinking water over the second half of the nineteenth century gradually helped to stop the incidence of cholera epidemics. The last major one seems to have been in 1866. A report from Dublin’s Mater Hospital in that year reads:
Dublin – this city received its first case of cholera in the person of a young woman named Magee, who imported the disease from Liverpool into No. 22, City Quay, from which point it spread all over Dublin and the suburban towns, ‘destroying in six months 1193 persons’.[15]
Treating smallpox
The later decades of the 19th century also saw massive progress made in vaccinations that eventually eliminated smallpox.
In the 1850s smallpox was killing about 1,500 people in Ireland every year, but by 1867 this was down to just 20 and by the 1890s the Irish health authorities claimed that Ireland had ‘totally immunity’ to smallpox. [16]
Smallpox was all but eliminated by vaccinations in the 1860s.
This was as a result of an 1863 law (following one in England and Wales in 1853) making vaccination of infants against smallpox compulsory. [17] Indeed vaccinations in Ireland, which were administered via the Poor Law Unions and Dispensaries – which amounted to the public health system at the time – appear to have been more successful in Ireland than in Britain itself.
In 1871 a smallpox epidemic broke out in Britain, killing over 45,000 people but causing just under 4,000 deaths in Ireland 1871, mostly, one assumes, among those who had not been vaccinated.[18]
And while it was not true as the Poor Law Commissioners claimed in the 1890s that Ireland had ‘total immunity’ to smallpox – there was for instance an outbreak in Dublin in 1903 that claimed 33 lives[19] – the disease was well under control, due to vaccination, by the second decade of the twentieth century.
There was a smallpox scare in in Ireland in 1966 due to an outbreak in Wales, but by 1980 smallpox had been declared eradicated worldwide.
The 1918 pandemic
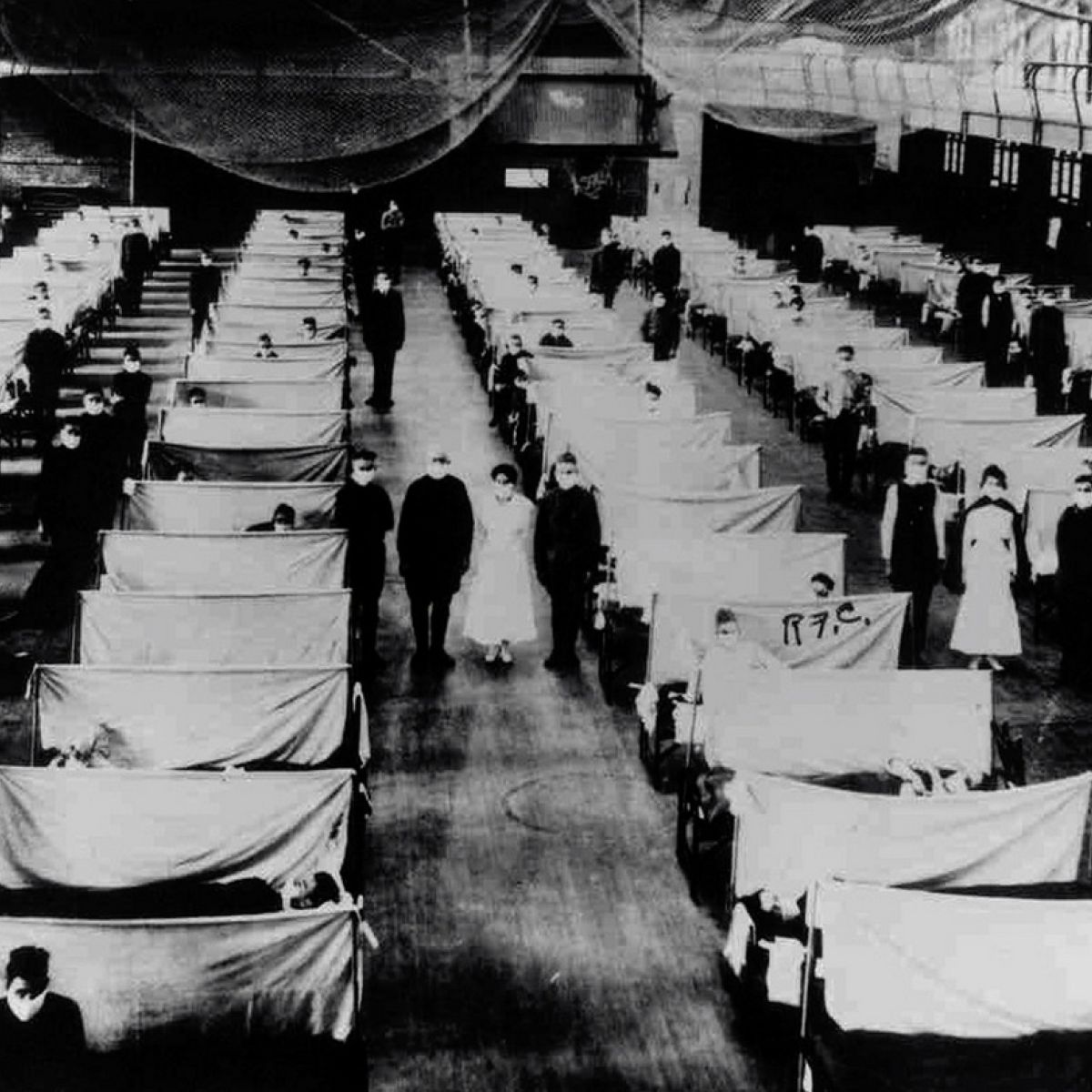
There is not space here to deal with the 1918 flu epidemic in depth. Readers are referred to Ida Milne’s recent ‘Stacking the Coffins’ and Catriona Foley’s ‘The Last Irish Plague’ for its impact on Ireland.
Suffice to say that the H1N1 virus, thought to have passed from poultry to humans in military camps during the First World War, spread around the world in late 1918-19 and killed perhaps 50 million people worldwide.
In Ireland it infected some 800,000 people or about 20 per cent of the population and killed at least 23,000, mostly from October 1918 to February 1919.
One important difference between the 1918 flu and the current Coronavirus epidemic is that while the latter primarily kills the old and sick, the former particularly killed the young and healthy in disproportionate numbers.
The 1918 pandemic infected over 800,000 people in Ireland and killed over 23,000. It provides important lessons for today.
However there are a number of important lessons that can be applied from the 1918 pandemic to today’s situation. Firstly, the importance of identifying and isolating cases. Republican activist and doctor Kathleen Lynn complained that the disease was spread by the failure to quarantine sick soldiers who had returned from the war fronts. And in hindsight she was quite correct. The areas with the heaviest mortality – included not only cities such as Dublin and Belfast but also rural areas such as Kildare and Donegal, which all had a heavy military presence.
Secondly, the professions most likely to die in the 1918 epidemic were doctors, nurses and policemen, highlighting the urgent need for protective equipment for such people. Today at least one in four of the cases of Covid 19 in Ireland are health workers.
Thirdly, the 1918 pandemic highlights the importance of ‘joined up’ strategic healthcare. In 1918 there was no national health authority either in the United Kingdom as a whole or in Ireland in particular. Rather health was the responsibility of local health boards under the Department of Local Government. This situation continued in independent Ireland until the creation of the Department of Health in 1947.
The result was that different measures were taken in different places. Thus while Limerick city for instance closed theatres and cinemas, Dublin did not – though Charles Cameron the head of Dublin public health department had them and the city’s trams, cleaned and disinfected every night. Schools were closed and sporting events suspended, but campaigning for the December 1918 general election, including mass rallies, went ahead, as did the election itself, which must have contributed to the spread of infection.
The most effective response to the epidemic seem to have been from activist and philanthropic groups rather than Local Government Boards, many of whom moved too slowly to tackle the outbreak. This should be borne in mind given that in 2020 there are two jurisdictions on the island with two divergent strategies for dealing with the epidemic.[20]
The pandemic of 1918 was the last mass mortality epidemic in Irish history to date. Though Ireland was impacted by the influenza pandemics of 1957 and 1968, they do not seem to have caused large excess mortality here.
Tuberculosis and Polio
Furthermore, the second half of the twentieth century is actually a story of great progress in the field of public health.
Polio, a virus that can cause paralysis and death, was known in infants for many centuries, but only became prevalent among adults after 1900, one victim being 1916 revolutionary Sean McDermott. It became more common in the 1920s and 30s and became notifiable disease (meaning that it was compulsory to notify the authorities of cases) in Ireland in 1941. There were outbreaks causing hundreds of deaths in 1947, 1950, 1953 and (localised to Cork) in 1956. [21]
Those seriously affected often had to be ventilated in what was at the time known as the ‘iron lung’. And those who survived were often left crippled.
However, by the late 1950s the disease had been all but eliminated by an extensive vaccination programme.
The story of the second half of the twentieth century is of great progress in medical science. In Ireland both tuberculosis and polio were eliminated by vaccination.
Similarly Tuberculosis, a disease that routinely killed about 4-5000 people every year in late nineteenth and early twentieth century Ireland, was finally brought under control in the early 1950s. Again, vaccination played a major role in this, but so too did common sense medical measures when properly funded.
Anne MacEllen writes of the approach of doctor Dorothy Price to the disease, ‘she believed that early accurate diagnosis, followed by isolation from the source of the disease along with bed rest were essential for recovery.’ Price was appointed chairwoman of a National Consultative Council on Tuberculosis by health minister Noel Brown in 1948.[22]
By treating patients in well run sanatoriums, use of anti-biotics for treatment and vaccination against the disease, tuberculosis had effectively been eliminated as a major health risk in Ireland by the late 1950s.
This article is being written in uncertain times. The Irish government has taken early measures to combat the spread of the coronavirus that will hopefully be effective. Historical experience shows that even in the absence of cure or vaccine, suppression measures, as well as general good hygiene, can be effective at limiting and suppressing epidemics. And that once a vaccine is developed, as it will be, the virus can rapidly be brought under control.
But the public must heed the directives of the healthcare authorities and those health workers confronting the epidemic must be given the protection they need.
References
[1] https://www.libraryireland.com/IrishPlaceNames/Tallaght.php
[2] Maria Kelly, History Ireland, 2001, Unheard of Mortality, the Black Death in Ireland. https://www.historyireland.com/medieval-history-pre-1500/unheard-of-mortality-the-black-death-in-ireland/
[3] Sean Duffy, Ireland in the Middle Ages, p.151
[4] Colm Lennon Sixteenth Century Ireland, p. 8
[5] Lennon, p.27
[6] Laurence Geary, Epidemic Diseases of the Great Famine, History Ireland, Spring 1996. https://www.historyireland.com/18th-19th-century-history/epidemic-diseases-of-the-great-famine/
[7] Geary, Epidemic Diseases of the Great Famine.
[8] Dean Ruxton, Irish Times 15 March 2020. https://www.irishtimes.com/news/ireland/irish-news/wakes-beggars-and-bad-air-when-typhus-killed-65-000-people-in-ireland-1.4203488
[9] Cormac O Grada, Black 47, p92
[10] Geary Epidemic Diseases of the Great Famine
[11] O Grada, Black 47, p.95
[12] Ibid. p.95-96
[13] The Battle to get rid of Irish Typhus, Dr Patrick Rowan, Irish Medical Times October 2009. https://www.imt.ie/opinion/guest-posts/the-battle-to-get-rid-of-irish-typhus-28-10-2009/
[14] Geary, Epidemic Diseases of the Great Famine, O Grada, Black 47, p.178
[15] Mater Hospital Report, August-December 1866 https://collections.nlm.nih.gov/catalog/nlm:nlmuid-34720790R-bk
[16] Deborah Brunton, The Problems of Implementation, The failure and success of small pox vaccination in Ireland 1840-1873. In Medicine, Disease and the State in Ireland, 1650-1940, edited by Greta Jones, Elizabeth Malcolm, p.138
[17]Brunton, p.149
[18] Ibid. p138
[19] https://www.dublincity.ie/image/libraries/dd004-smallpox-hospital
[20] For sources on the 1918 epidemic see Milne, Stacking the Coffins, Foley the Last Irish Plague, On Dublin, Padriag Yeates, Dublin A City in Wartime 1914-1918, p270-275. For Limerick see, Des Ryan, The Great Influenza Epidemic 1918-1919, Old Limerick Journal Winter 1996 http://www.limerickcity.ie/media/Media,4106,en.pdf For an overview online see, Guy Biener, Patricia Marsh, Ida Milne, History Ireland 2009, https://www.historyireland.com/20th-century-contemporary-history/greatest-killer-of-the-twentieth-century-the-great-flu-of-1918-19/
[21] Laurence Geary, The 1956 Polio Epidemic Cork. History Ireland May June 2006. https://www.historyireland.com/20th-century-contemporary-history/the-1956-polio-epidemic-in-cork/.
[22] Anne MacLellan, Dorothy Stopford Price and the Tuberculosis Epidemic https://dh.tcd.ie/pricediary/about-dorothy-price-her-family/dorothy-stopford-price-and-the-irish-tuberculosis-epidemic/